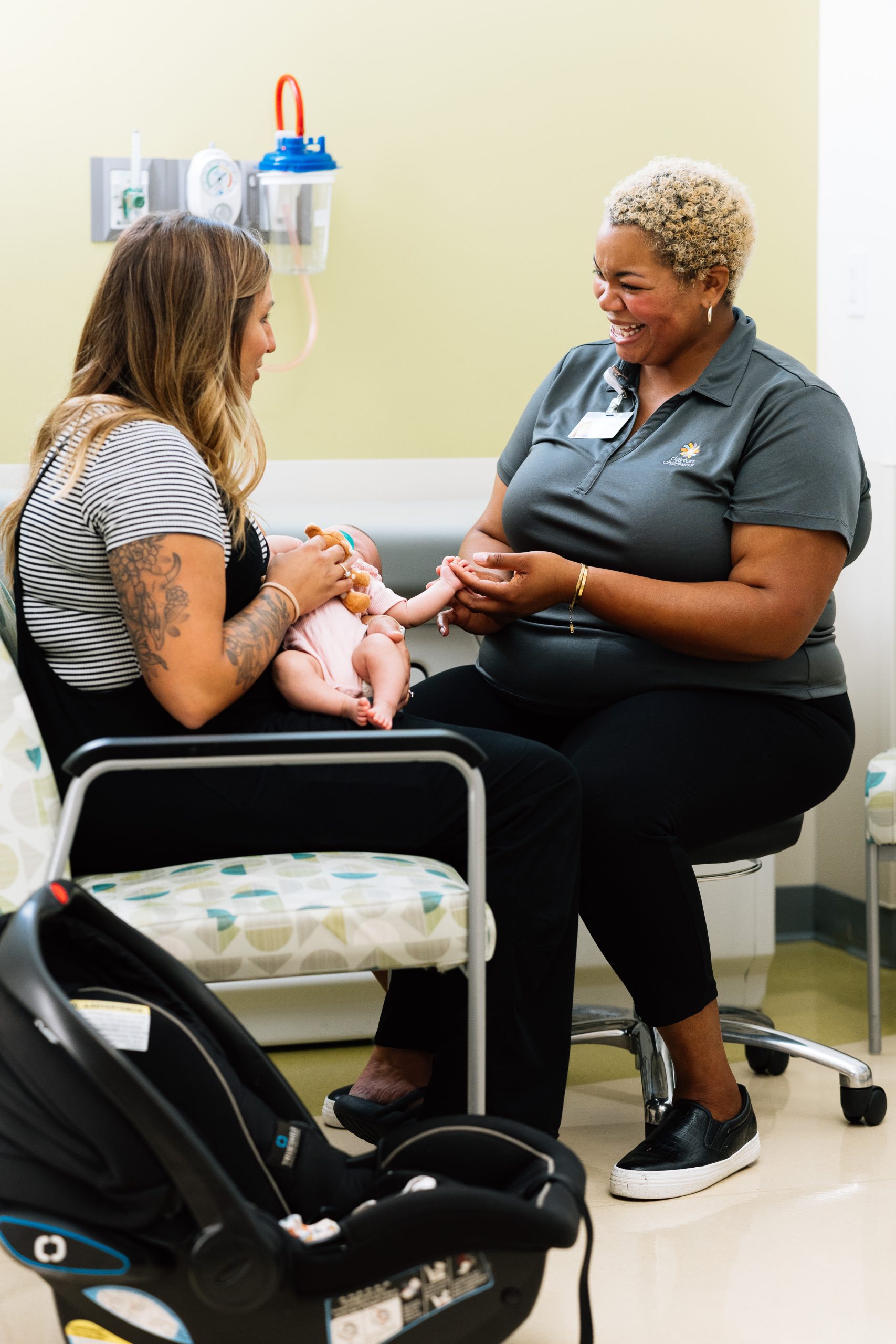
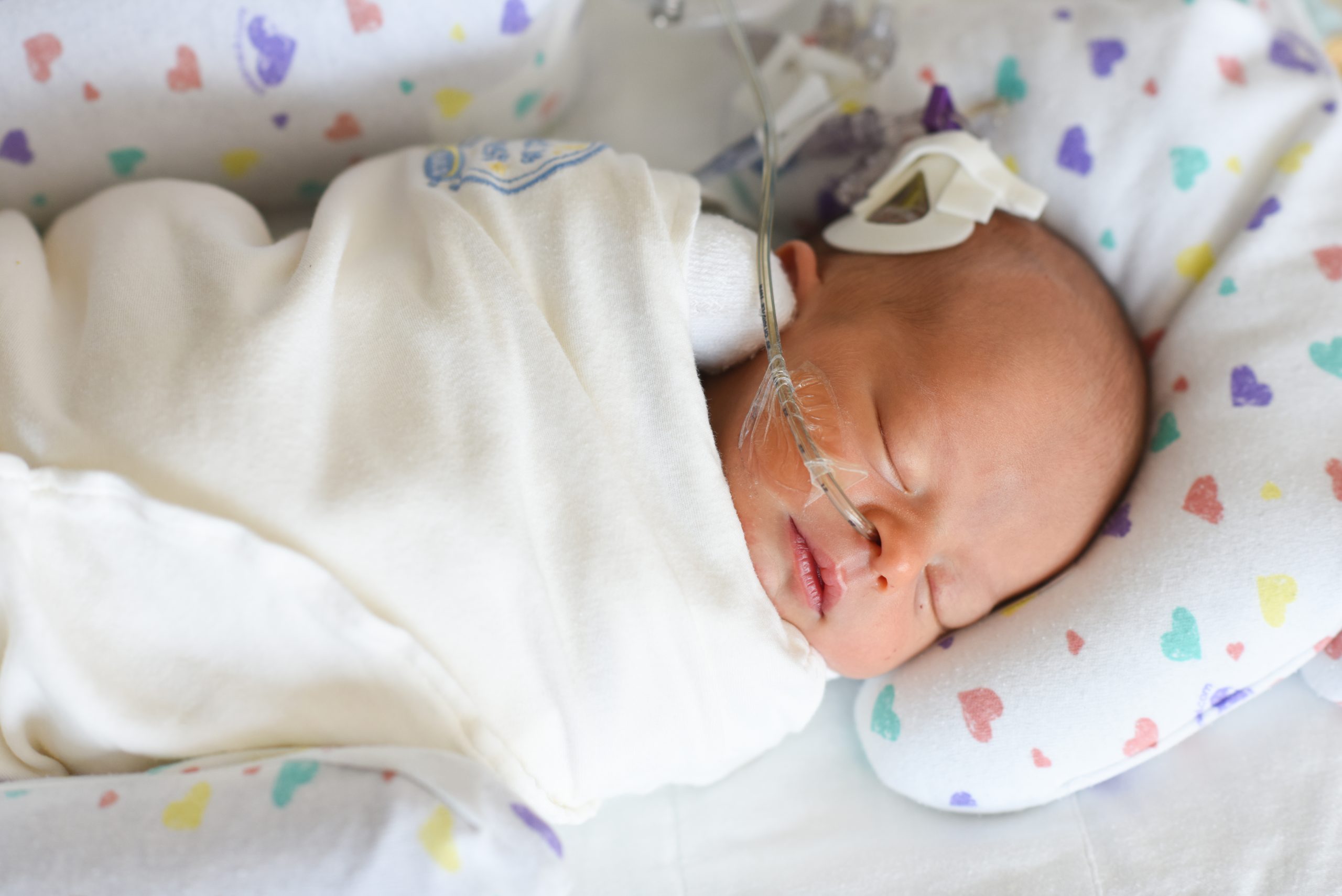
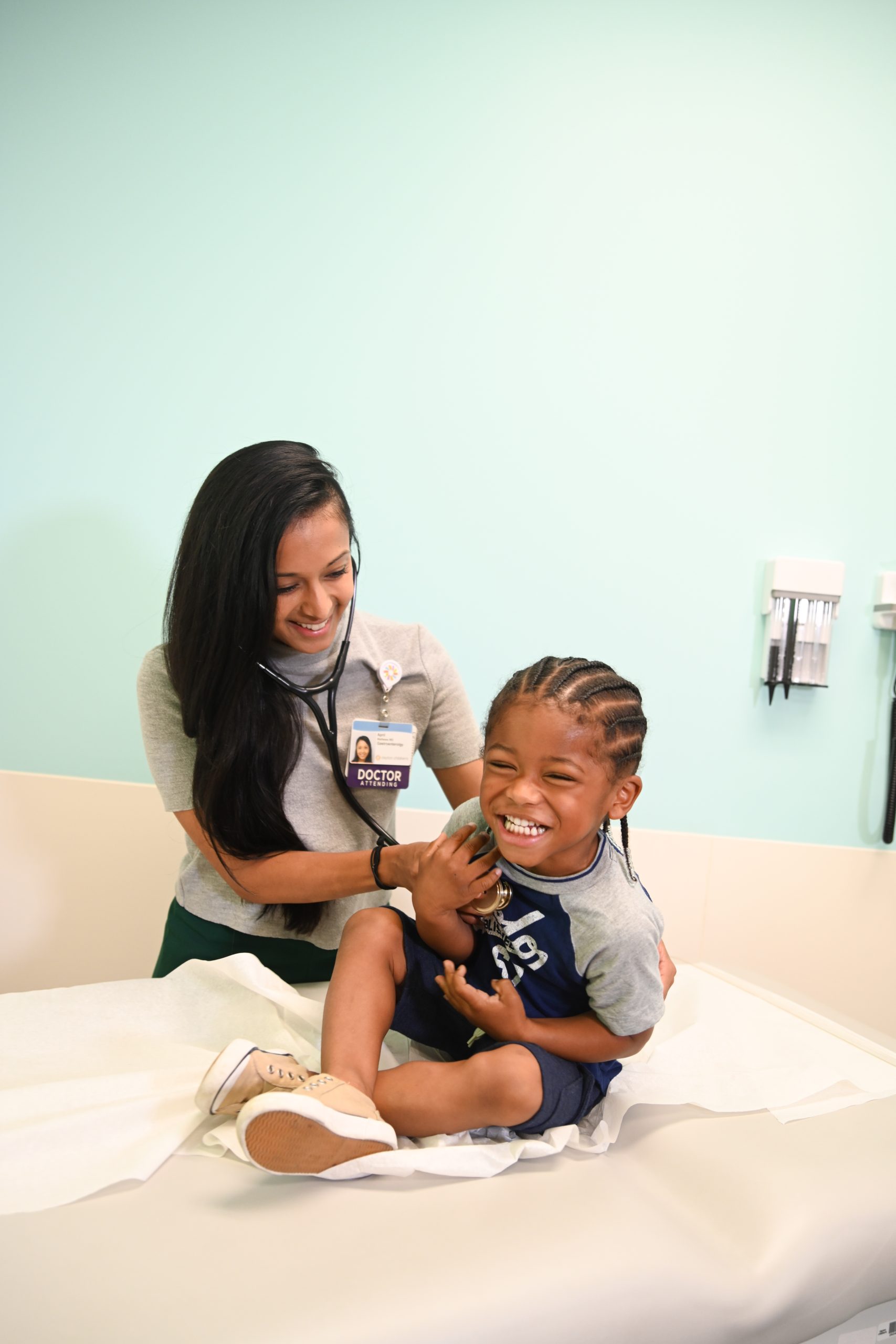
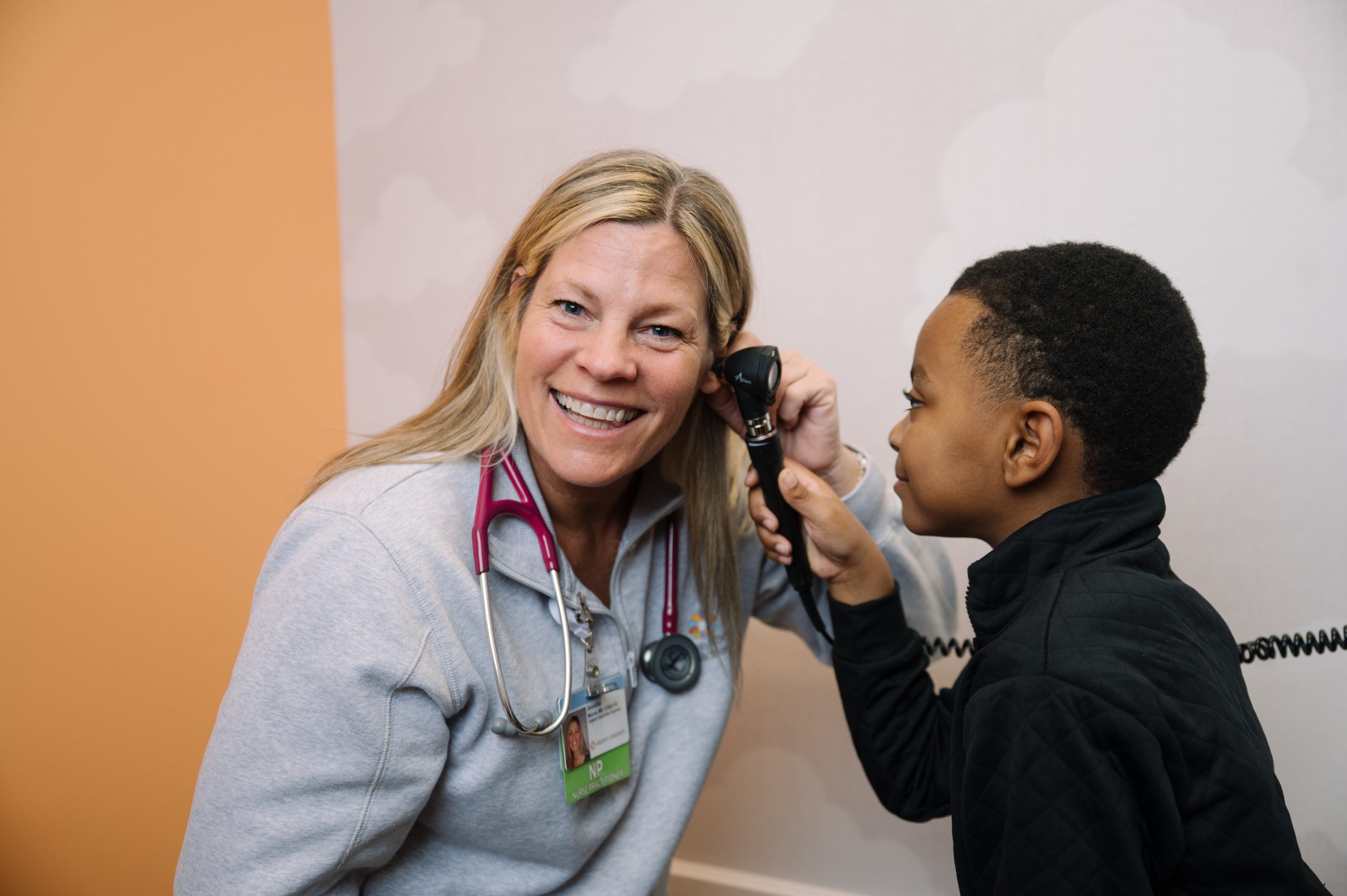
why does this gift matter?
Too many children only enter the health system in moments of crisis. Families face barriers in access to care; mental health needs go unmet until they escalate, and care is often fragmented across settings. Even with world-class hospitals, outcomes for our children remain poor:
- Ohio routinely ranks in the bottom half of states on many child health measures, despite having some of the nation’s leading children’s hospitals.1,2
- In our region, one in three children younger than 15 months don’t get their recommended well-child visits, 3 creating significant gaps in preventive care that can delay diagnosis, allow concerns to escalate, and ultimately lead to poorer health and developmental outcomes. These missed touchpoints are especially consequential as early identification is critical for addressing emerging physical, behavioral, and mental health needs.
- Nationally, 60% of kids who die by suicide never got a mental health diagnosis, meaning they never got to the right care when it was needed.4 Prevention and early intervention—particularly those focused on youth mental health—are essential to reversing the current crisis but remain difficult to sustain due to high operating costs and chronically inadequate reimbursement.
Many prevention-oriented and access-focused programs receive limited or no reimbursement at all, despite their proven value. Evidence consistently shows that earlier access to timely, local care improves outcomes by enabling faster intervention, stabilizing issues before they worsen, and reducing reliance on more intensive and higher cost treatments later.
Sources: